We are delighted and honoured to have been invited to pump prime neonatal training in Murambinda Mission Hospital, Zimbabwe. Teaching equipment is all packed up, printing and laminated completed, visas and malaria pills procured; ready for the off! 5 international instructors are travelling to Zimbabwe from Cameroon, Uganda and UK to teach the first 2 NCCs with a view to facilitating the first instructor training course at the end of 2026. Funding for the programme is from Friends of Murambinda (About us – Friends of Murambinda Hospital UK Charity 1073978), a small charity run by previous volunteers at the hospital.
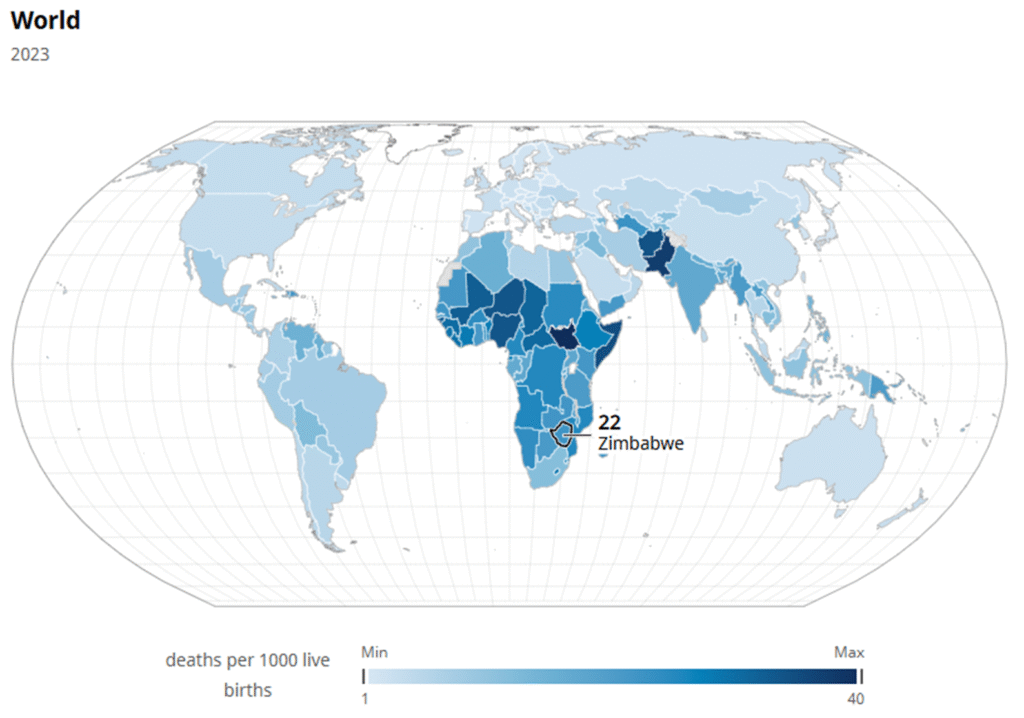
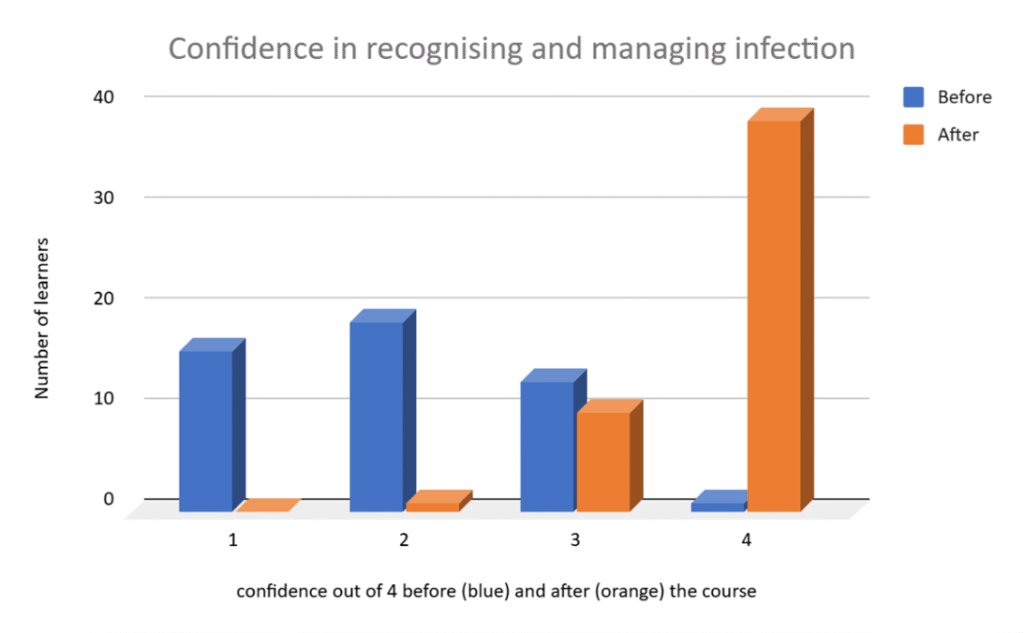
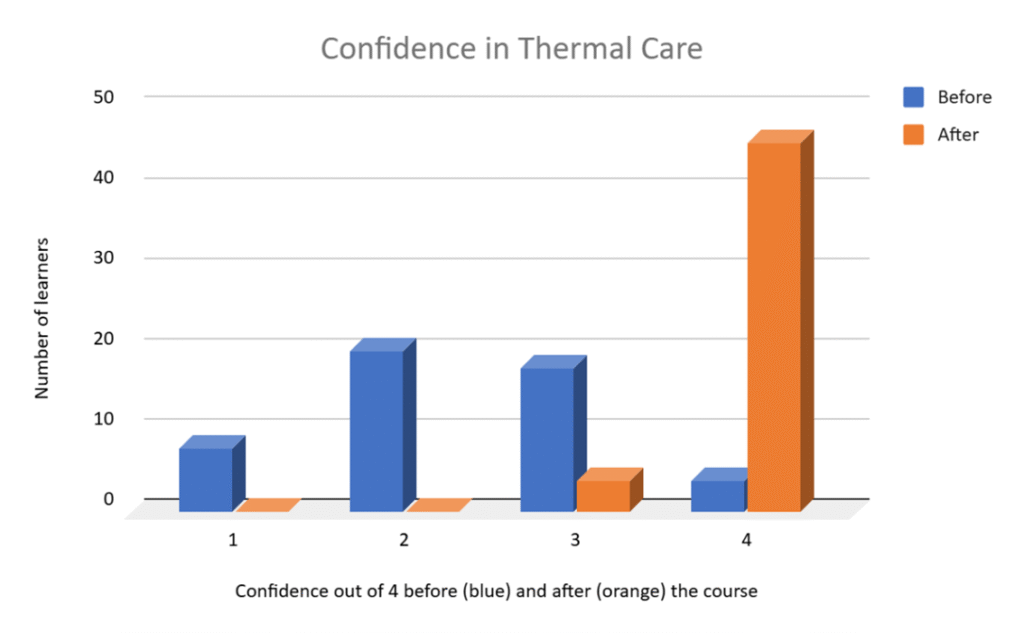
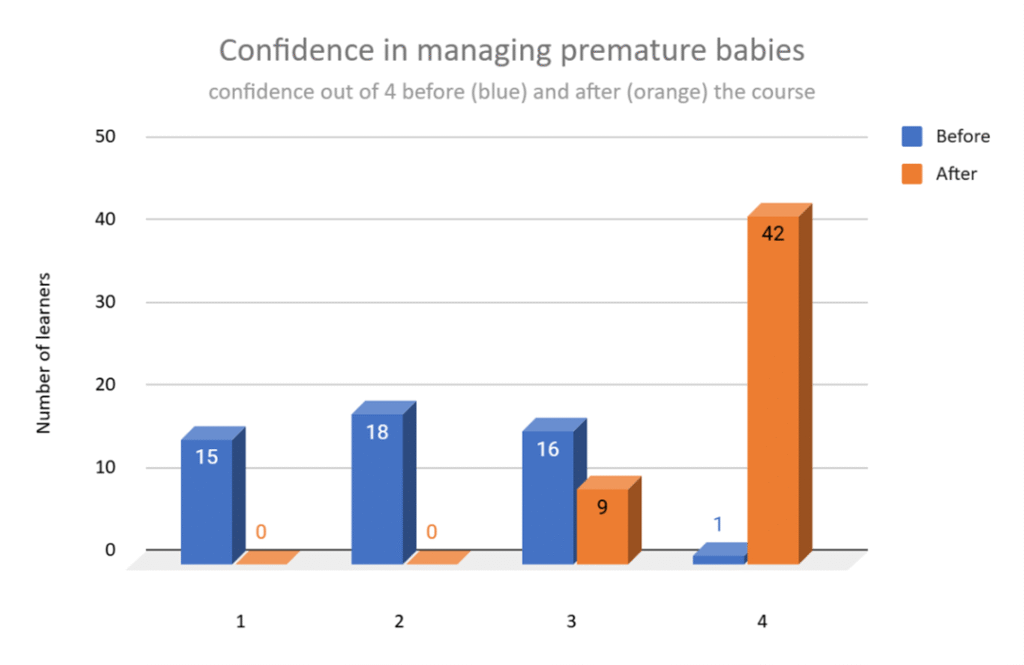
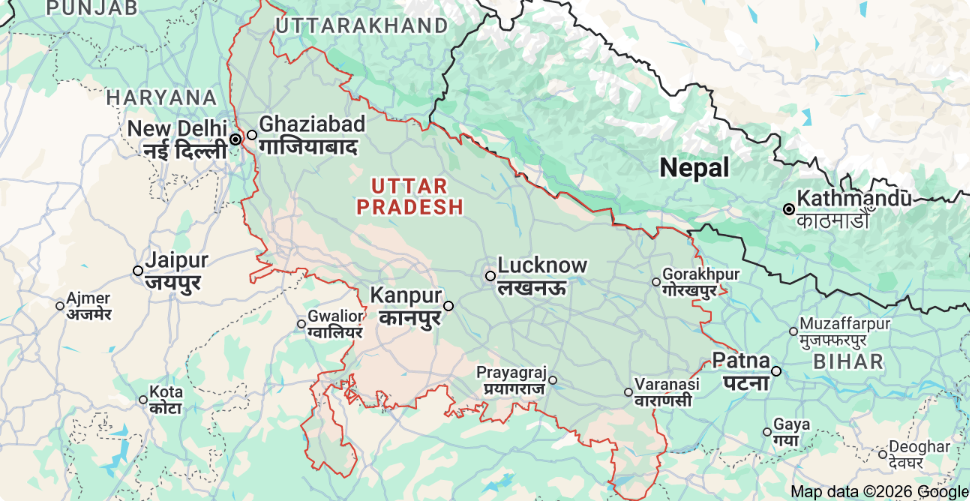
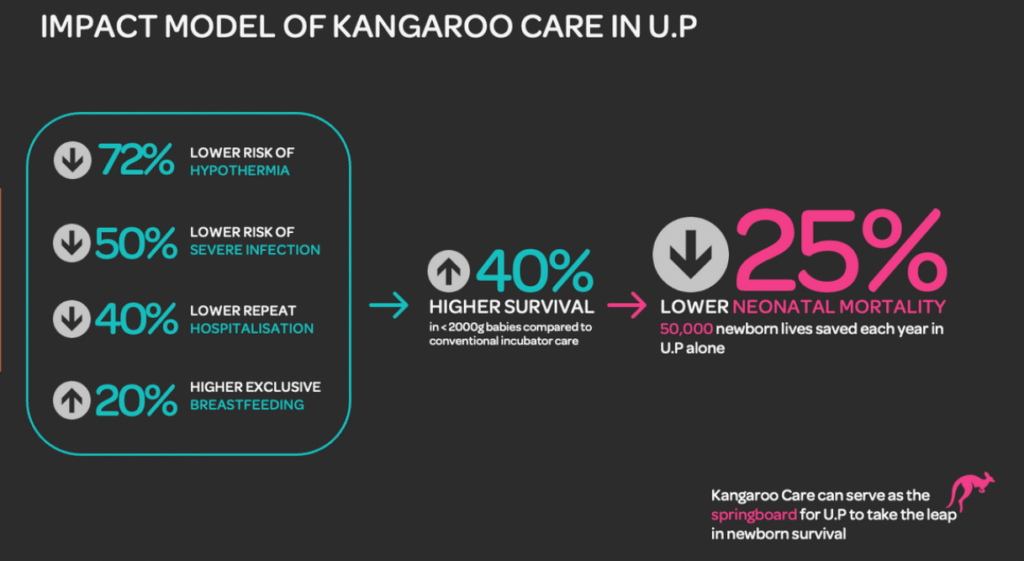
Zimbabwe’s neonatal mortality rate figures range from 22 per 1000 live births to 30, depending on the information source. Interestingly, the proportion of deaths attributed to premature birth is higher in Zimbabwe than the world averages and those caused by sepsis therefore make up a smaller proportion. In reality, many preterm births are caused by infection so there is inevitably a bit of crossover in the classification. Fortunately, the Neonatal Care Course contains a lot of material about keeping preterm babies warm and feeding them as well as revamped sessions on recognition and management of sepsis.